Heart Health
Heart Health
The Role of Luteolin in Preventing Arterial Plaque
Understanding the mechanisms and potential benefits Arterial plaque, a major contributor to cardiovascular diseases, results from the accumulation of fatty deposits, cholesterol, and cellular waste products in the walls of arteries. Over time, these plaques can...
A New Weapon for Beating Heart Disease
Heart disease is the number one killer of men who are otherwise living an energetic, productive life. Often the first symptom of Heart (Cardiovascular) Disease is a Heart Attack resulting in sudden death from blockage of one of the Coronary Arteries supplying blood to...
Icariin – Potential Super Supplement: Good For Everything?
Aging is accompanied by rising pain levels in practically everything in our bodies. Mine happens to be focused on knees and neck. That recently sent me to look into the ingredients of the well-advertised "Relief Factor". Of the four ingredients, the only one I was not...
Battling Artery Disease and Stent Restenoisis
I figured out that I had coronary artery disease (CAD) back in 2000, and received a 4-way bypass operation in late January 2001. That's what really prompted the creation of the SeniorFitness.com website; I wanted to pass on whatever I learned about how I clogged my...
Osteoporosis and Heart disease; Vitamin K2 Looks to be the Cure for Both
Hi All - In the years I have been researching to find the cause of my heart disease and how to reverse it, I've found nothing more incidental to the disease process than vitamin K2 deficiency. Vitamin K2 looks to be the missing link to both cause and reversal. I have...
Good News on the Heart Disease Front
I have had a battle with coronary artery disease, resulting in a quad bypass in 2001 and now stents in 2014. I have been looking for the real cause for a long time to avoid further problems. Now I have another insight that I think will make a big improvement; but...
Heart surgeon declares on what really causes heart illness
By Dr. Dwight Lundell Dec 8, 2013 - We physicians, with all our experience, know how and authority often acquire a rather large selfishness that tends to make it hard to accept we are wrong. So, here it is. I openly admit to being mistaken. As a heart surgeon with 25...
Belly Fat May Hit Your Heart the Hardest
By Steven Reinberg Frank's Comments: OK - this is yet another article backing the idea that the fastest way to beat metabolic syndrome and type-II diabetes is to build muscle while relearning how to eat correctly for true health. What is needed is a serious, high...
Avoiding Heart Disease for Life
-esFor decades now the cardiologists have been telling us that the single-most important factor in heart/vascular disease is our Low Density Lipoprotein Cholesterol (LDL) count. For almost as long the awareness has been building that oxidized LDL is the stuff that...
A Controversial Perspective on Nutrition
I've had a recent jolt to my understanding of nutrition, particularly with regard to fats and oils. I went looking for a private gym to see if I could do a joint venture and film some training videos with the owners. One of them took a look at my writings and website...
I have heart disease, so this is personal!
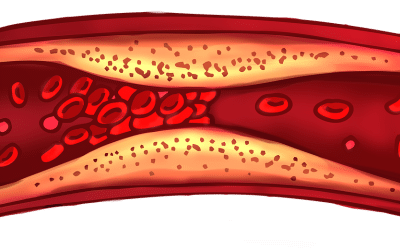
For the last 15 years I have been researching the literature for the causes for atherosclerosis(the name for plaque buildup in arteries), and there are many, but the science of the disease has become more clear in the last few years. Still, there is considerable disagreement among authorities about the actual causes and the best strategies to avoid or heal the disease. In this category I attempt to present the known causes and strategies for avoiding or living with this disease.
The plaque-building process starts at a young age
Arterial Plaque has historically been seen in autopsies of young, deceased soldiers in our national conflicts and wars. Arterial health has improved over the last few generations, so atherosclerosis rates seen in soldiers in Korea, Vietnam and Iraq/Afghanistan has declined respectively: 77%, 44% and 8.5%. Part of this reduction is attributed to reduction in smoking rates, but also on other lifestyle and nutrition changes. [1] The point is that the process starts in youth, often long before we see any rise in blood pressure or cholesterol levels, so strategies for prevention need to be inculcated at a young age for the best outcomes.
However, atherosclerosis is considered a “disease of aging” and its progression accelerates with aging and becomes symptomatic typically in middle age and beyond. Most of the factors involved in this acceleration are discussed in this study reference. [2] The study points to cellular senescence (cells getting old and ceasing to function well) as a major factor, and details several mechanisms by which the cells involved in artery structure get old and add to the disease progress. It offers some thoughts on prevention or healing, but mostly clarifies what goes wrong unseen in our arteries.
Aged endothelial cells (ECs) and aged vascular smooth muscle cells (VSMCs) make arteries stiffer, raise blood pressure, raise vascular inflammation, encourage the formation of arterial plaque and speed up the closing down of arteries as seen in coronary artery disease. This is a very informative study – if you can wade through it; it’s well worth reading. The basic message is this: whatever we can do to slow cellular aging will also reduce the speed at which atherosclerosis progresses.
Do you see a disconnect here? Aging may accelerate the final stages of the disease, but it can’t be the cause of it because it starts in youth. We need to know what initiates the process in the first place and eliminate the cause, and we need to know how to reverse the process if it has started in our past.
Tobacco Smoking:
“In conclusion, smoking can cause production of dysfunctional lipoproteins having a smaller particle size that exacerbate senescence and atherogenic progress due to oxidation and glycation.”[3]
Lipoproteins – How Fats Move Through Our Blood System (remember that oil and water don’t mix)
The liver initially makes VLDL as the empty carrier for various fats and then, as the liver is the primary processor of all dietary fats, it packages fats into these particles at various densities, depending on their purpose and sends them into the blood stream for transport. The liver also makes HDL particles, also made by the cells lining the intestines, which are empty of any form of cholesterol.
HDL is different in that it is involved in bringing unused fats back to the liver and also functions as an antioxidant in the process. When it returns cholesterol from the body, that is called Reverse Cholesterol Transport, and is the primary way that HDL reduces or prevents arterial plaque buildup. [4]
For many decades science has mistakenly thought that the more LDL we produced, the faster our arteries plug up; but the process proves to be much more complex. Under a variety of stress conditions, our liver can make smaller, more dense lipoproteins, primarily LDLs, which are dysfunctional in that they can be easily damaged.
Damaged LDLs become invasive in the artery walls, burrowing under the endothelial cells lining all arteries, creating local inflammation that brings immune cells into the artery wall which become part of the plaque. The question now being settled is whether immune cells are first attracted to damaged LDLs (and other damaged lipoprotein elements) and then invade the artery lining, or rather are gobbled up by immune cells which then burrow into the artery wall?
The starting point for prevention of heart disease, it seems to me, is to understand how dyslipidemia gets started in the first place.
Causes of Dyslipdemia
Hypothyroidism and Dyslipidemia
Hypothyroidism is the most common pathologic hormone deficiency among the endocrine disorders. It is characterized by declining levels of thyroid hormones T4 and T3, with rising TSH. Hypothyroidism may be due to primary disease of the thyroid gland itself or hypo-secretion of the pituitary TSH. Thyroid hormones have significant effects on synthesis, mobilization and metabolism of lipids. Overt hypothyroidism is associated with elevated cholesterol, but more importantly, with elevated levels of small-dense LDL (sdLDL) and oxidized LDL (oxLDL), which are proving to be causative factors in artery disease initiation and progression. [5]
It remains to be seen whether thyroid deficiency is a primary initiating cause of dyslipidemia, but the latest research shows that it is a contributing factor.
Metabolic Syndrome and Dyslipidemia
The latest science has led to this conclusion; metabolic syndrome is caused by excess food intake over a long time period, during which these metabolic malfunctions manifest and worsen. It is hastened by eating high-glycemic foods that excessively and repeatedly raise blood sugar until insulin receptors in many of our tissues and organs become insensitive to insulin and glucose levels in the blood remain constantly elevated.
This study cited above shows that the primary mechanisms that damage LDL are oxidation and glycation, and these encourage it to invade artery walls and build plaque. It is important to understand that these same mechanisms (oxidation and glycation) are inflicting damage in every body; they just damage us much faster if we smoke or eat a diet that leads us to have chronically high blood sugar.
Oxidation:
When oxidized, these particles attract immune cells (monocyte-derived macrophages) which engulf these damaged lipoproteins and are prone to invade our artery structures, become foam cells, leading to plaque formation. HDL prevents plaque formation by binding to macrophages and removing the damaged cholesterol, both in circulating blood plasma and in the space below the endothelium in the artery walls [6].
More to come – work in process.